THE SCIENCE OF INFLAMMATION RESET
Understanding & Addressing the Root Cause of Modern Disease
Chronic Inflammation: The Silent Driver of Most Chronic Disease
Chronic inflammation is now recognized as a participant in—or cause of—most chronic disease known to humankind1. It is estimated that over half, and possibly as much as 70% or more, of all deaths involve diseases either caused or worsened by chronic inflammation2.
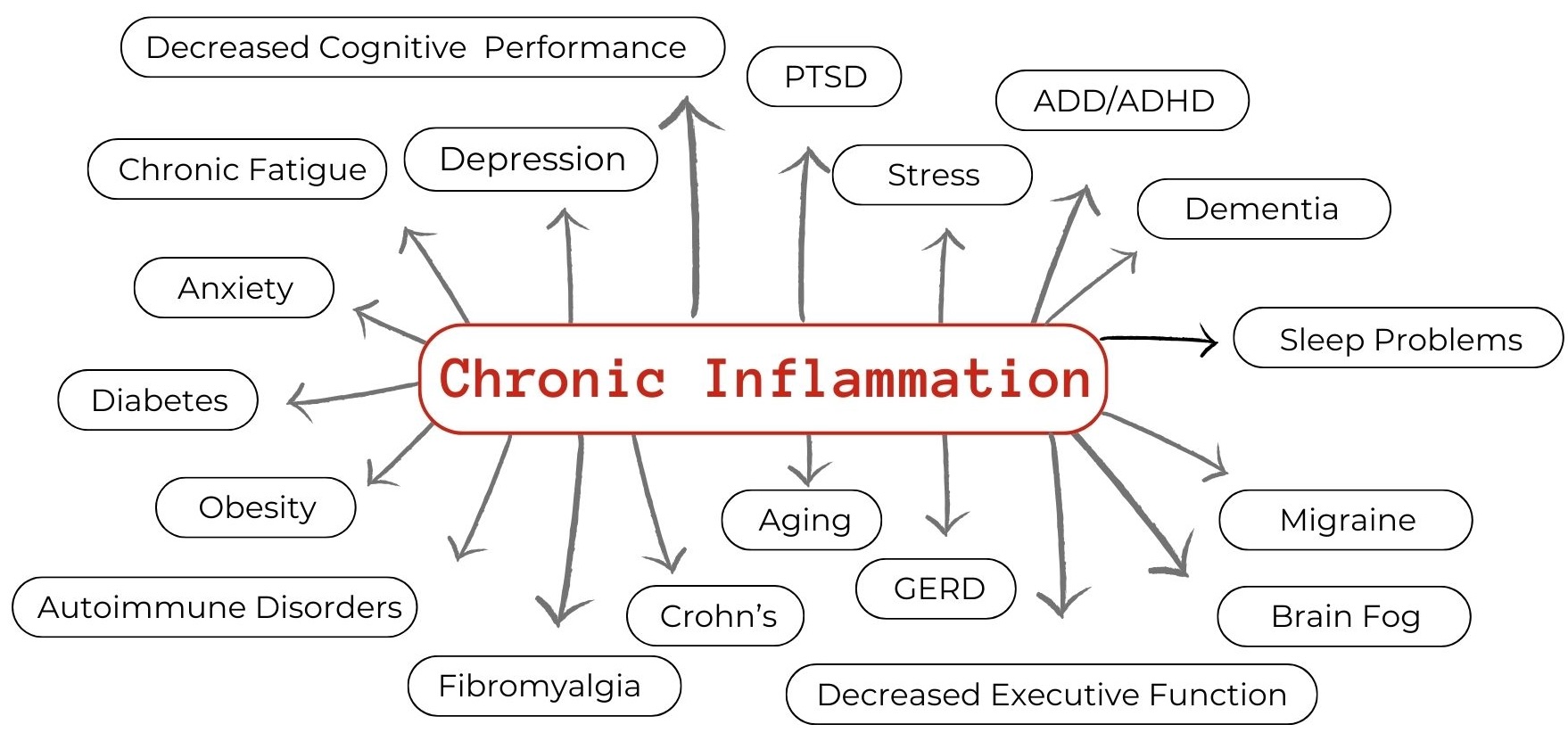
The Inflammatory Link to Mental Health
Inflammation affects more than just physical health—it plays a critical role in mental well-being and cognitive function. Studies link chronic inflammation to a variety of mental health challenges, including: depression, anxiety, ADHD, PTSD, dementia, and neurodegenerative conditions3.
Emerging research suggests that dietary interventions can be as effective as conventional therapies in improving outcomes for many mental health conditions4,5.
"Inflammaging" Drives Aging6
Inflammation accelerates the biological aging process, a phenomenon called 'inflammaging.' This explains why some people experience faster declines in energy, cognitive function, and tissue regeneration. Inflammaging affects multiple systems in the body:
Cellular Energy Production: Damages mitochondria, reducing the body’s ability to generate energy.
DNA Repair & Longevity: Increases genetic instability, accelerating biological aging.
Tissue Regeneration: Slows the body’s ability to repair damaged cells and tissues.
Metabolic Health: Disrupts insulin sensitivity, increasing the risk of metabolic disorders.
Immune Resilience: Weakens the immune system, increasing susceptibility to infections and age-related illnesses.
Inflammation Affects Executive Function, Focus, and Productivity7, 8,9
Even low-level inflammation has been shown to directly affect brain function and cognitive performance. Research shows elevated inflammatory markers like C-reactive protein (CRP) and interleukin-6 (IL-6) correlate with:
Reduced memory, learning, and executive function.
Slower decision making.
Poorer focus and presence.
Decreased motivation and drive.
Heightened stress reactivity and fatigue.
These effects aren’t just short-term—they contribute to long-term cognitive decline and hinder productivity.
The Hidden Impact of Sub-Clinical Inflammation
Even without diagnosed conditions or elevated biomarkers, low-level inflammation can silently affect how you feel and perform. Common signs include unexplained:
Fatigue or energy dips.
Brain fog or reduced mental clarity.
Mood swings.
Decreased stress tolerance.
Digestive issues.
Sleep disruption.
Slower recovery from exercise.
Subtle joint or muscle discomfort.
Take Action to Clear Inflammation
The good news is that many people have successfully cleared inflammation from their bodies and reclaimed their health. Understanding inflammation’s role is the first step. The next is taking precise, personalized action to clear it.
The Art and Science of Clearing Chronic Inflammation
Our Bodies Are Designed for Balance
Although it may not feel like it when struggling with a chronic illness or autoimmune disorder, the human body is a master of homeostasis—constantly adjusting to maintain equilibrium across energy production, metabolism, immune function, and cellular repair. Whether we realize it or not, there is generally more "health" in our bodies than there is disease or dis-ease at any given time.
Under normal conditions, inflammation is a temporary, adaptive response, helping the body heal from injury or infection, and restore balance. But when something goes awry in the normal healing process, chronic inflammation can become a central driver of chronic health and performance challenges.
Acute inflammation is short-term, protective, and resolves once healing is complete.
Chronic inflammation lingers, misfiring even in the absence of infection or injury, creating widespread dysfunction.
We Do Not Currently Live Under Normal Conditions.
Our modern lifestyle has quite literally disconnected us from our natural relationship with the Earth—modern conveniences and diets, shoes, medications, environmental toxins, light and noise pollution, poor sleep, and persistent psychological stress—all disrupt our body’s natural ability to maintain equilibrium. Most of us spend our days physically removed from nature:
We primarily walk on artificial surfaces in rubber-soled shoes, and rarely touch the Earth.
Most of us expose ourselves to blue-light emitting screens (TV, computers, phones), which disrupts our circadian rhythm and melatonin production.
We spend most of our time indoors, lacking exposure to natural sunlight, which is critical for immune function, hormone regulation, and inflammation control.
We are constantly exposed to EMF and WiFi frequencies, which have been shown to affect cellular health and promote inflammation.
At the same time, industrial agriculture and modern food production have fundamentally altered our food supply, exposing us to inflammatory triggers from field to fork:
Soil Depletion & Nutrient Loss → Industrial farming and monocropping have stripped farmland of essential nutrients, leading to a severe decline in food nutrient density.
Pesticides & Chemical Residues → Pesticides and herbicides contaminate soils, air, and water and remain on the foods we eat.
Factory-Farmed Meat & Antibiotics → The widespread use of antibiotics and grain-based feed in livestock disrupts both human and animal microbiomes, increasing inflammatory risk.
Toxins in Food Storage & Processing → Mass food storage conditions create ideal environments for molds and fungal toxins, which can trigger immune responses and inflammation.
Hidden Chemicals in Foods and Food Packaging → Many endocrine-disrupting chemicals (EDCs) and plastics used in food packaging don’t even need to be disclosed on labels.
Ultra-Processed “Not Food” → Ultra-processed foods make up 67% of the American diet, driving gut dysbiosis, metabolic dysfunction, and systemic inflammation.
It is no wonder that even those who follow “healthy” lifestyles and diets often find themselves struggling with inflammation, fatigue, and chronic health challenges.
Clearing Inflammation in Today's World is Both an Art and a Science
Chronic inflammation is not an inevitability, and not everyone is inflamed to the point it affects their lives. But if you are inflamed or suffer from an inflammatory disease, and you are willing to action, it is possible to reduce inflammation, restore balance, and reclaim your energy and well-being.
"Let food be thy medicine, and let medicine be thy food"
~ Hippocrates
Food: A Foundational Approach to Addressing Inflammation
While many tools exist for managing inflammation—from medications to lifestyle interventions—food plays a central role in addressing inflammation. Research shows that one of the most effective ways to reduce inflammation in the body is through changes in diet10,11. This is why we advocate a Food First approach.

Food is Fundamental
Each meal directly interacts with your gut microbiome, immune system, and metabolic pathways.
Unlike supplements or therapies that work on the margins, dietary choices affect multiple aspects of health simultaneously.
Even the best anti-inflammatory interventions cannot overcome the effects of inflammatory foods.

Food is Frequent
We make food choices multiple times daily.
Each meal is an opportunity to support health.
These choices have cumulative effects on our inflammatory state.

Food is Biochemically Personal.
Not all "anti-inflammatory" foods work for everyone.
Many people unknowingly consume foods that trigger inflammation in their unique biochemistry.
Without personalization, even "healthy" foods can maintain inflammatory cycles.
Not All Anti-Inflammatory Diets Are Created Equal.
Many people turn to anti-inflammatory diets to reduce symptoms, improve energy, and restore balance. And for good reason—scientific research strongly supports the role of dietary interventions in reducing inflammation.
In fact, many of our clients come to us having already done an anti-inflammatory program with significant results—but they still feel like something is missing. They’ve made progress, but they haven’t quite crossed the finish line.
Why?
Inflammation is personal. The foods that reduce inflammation for one person may trigger it in another.
Most mainstream “anti-inflammatory” diets assume that all “healthy” foods work for everyone, but research shows that this is not the case. For some, salmon, blueberries, and lemon are powerful anti-inflammatory foods—while for others, they may contribute to low-grade inflammation or sensitivities.
Some people thrive on leafy greens and nuts, while others find that certain fibers, oxalates, or natural food compounds create discomfort or inflammatory flares.
Without a precise method to identify personal inflammatory triggers, many people experience frustration, stagnation, and unexpected flare-ups—even on diets marketed as anti-inflammatory.
The Emerging Science of Inflammatory Individuality
You, your biochemistry and your microbiome are unique, and what causes inflammation in one person does not cause inflammation in another.

While general diets often reduce inflammation for many people, most miss a vitally important point:
Your immune system, gut microbiome, metabolism, and genetic makeup are unique and that all plays a role in how your body processes different foods and environmental inputs.
This is why a one-size-fits-all approach to inflammation works only to a certain point.
What Determines Your Inflammatory Response?
Gut Microbiome Profile – The way your unique gut bacteria influence inflammation and immune signaling.
Immune Signature – Your immune system’s unique reaction patterns to foods, stressors, and environmental factors.
Metabolic & Hormonal Factors - Insulin sensitivity, cortisol levels, and metabolic health all impact how well your body processes nutrients and manages inflammation.
Lifestyle-Associated Molecular Patterns (LAMPs) – The cumulative effects of stress, sleep, and movement on inflammation resolution.
Inflammation is not only about food—it’s about how your body interacts with food.
The Optimal AF Bio-Specific Ultimate Inflammation Reset
Leading Edge Lab Testing
Once you understand that inflammation is personal and that food is the most fundamental way to clear it, the next step is to identify and eliminate the specific foods that trigger inflammation in your body.
This is where most anti-inflammatory diets fall short—they provide general guidelines but don’t account for your unique biochemistry. Or, they provide testing for inflammatory triggers but fail to provide a structured, scientifically validated process—the most effective way to clear inflammation and reset your body.
The Gold Standard of Elimination Diets
For decades, leading organizations such as the American Academy of Allergy, Asthma & Immunology (AAAAI) and The American College of Gastroenterology (ACG) have recognized elimination diets as the gold standard for identifying and reversing food-driven inflammation.
The gold standard elimination diet is the only clinically proven method to systematically remove inflammatory foods, reset the immune system, and reintroduce foods with precision to identify personal triggers.
At Optimal AF, we do both:
We use leading-edge lab testing to pinpoint your unique inflammatory triggers;
We then guide you through the gold standard of elimination protocols—the most effective way to clear inflammation and reset your system.
And, along the way, we teach you to experience how various foods affect your body, so you have the skills to maintain long-term health and performance.
Optimal AF is not a permanent diet. This is a six-month inflammation reset. Ultimately, the best diet is a more diverse diet—one that builds a resilient, dynamic microbiome, something that is lacking in industrialized countries.
How Optimal AF Works

Step 1: Identify Your Unique Inflammatory Triggers
We use leading-edge lab testing and clinical assessment to determine which foods are driving inflammation in your body.
This removes the trial-and-error approach of guessing which foods are safe.

Step 2: Systematically Remove & Reset
We guide you through the gold standard of elimination protocols, removing inflammatory foods while optimizing nutrient intake for healing.
This allows your body to reset inflammation pathways and restore balance.

Step 3: Reintroduce & Optimize Health
Once inflammation has cleared, foods are strategically reintroduced, helping you identify which foods support your health and performance—and which don’t.
This process teaches you to listen to your body, recognize subtle inflammatory responses, and build a sustainable, diverse diet that supports long-term health.
What to Expect from the Optimal AF Reset
1. The Journey to Reducing Inflammation is Both Individual and Gradual:
Initial changes in inflammation may be noticed within 4 - 10 days.
Sustainable results typically develop over 3-6 months.
Some people may need longer depending on their starting point.
Progress often occurs in layers rather than linearly.
2. Best Candidates for Success
This approach may be especially valuable if you:
Have tried other anti-inflammatory or dietary interventions with some success.
Are ready to make potentially difficult, temporary dietary changes.
Want to understand your personal inflammatory triggers.
Seek long-term solutions rather than quick fixes.
3. Working with Healthcare Providers
Optimal AF works best as part of a comprehensive approach to health:
We advocate a Food First approach, meaning we suggest you are willing and able to come off supplements, certain foods (e.g., coffee) and food groups (e.g., dairy) - Always consult a healthcare provider before making these changes.
We encourage maintaining relationships with healthcare providers.
Our program complements, rather than replaces, medical care.
Some conditions may require additional medical support, which we do not provide.
We can work alongside other therapeutic approaches and specific diets (e.g., low purine, low FODMAP, etc).
Unlike generic programs, the Optimal AF Reset is tailored to your unique biochemistry and needs.
Citations and Notes
Furman D, Campisi J, Verdin E, et al. Chronic inflammation in the etiology of disease across the life span. Nature Medicine. 2019;25(12):1822-1832.
Slavich GM. Understanding inflammation, its regulation, and relevance for health: A top scientific and public priority. Brain, Behavior, and Immunity. 2015;45:13-14.
Grau-Del Valle C, Tejada-Girbés J, Serra-Pérez M, et al. Association between gut microbiota and psychiatric disorders: A systematic review. Frontiers in Psychology. 2023;14:1215674.
Kobus-Cisowska J, Kusek M, Maruszczak J, et al. The role of gut microbiota in anxiety, depression, and other mental disorders as well as the protective effects of dietary components. Nutrients. 2023;15(14):3258.
Sarris J, Logan AC, Akbaraly TN, et al. Nutritional medicine as mainstream in psychiatry. The Lancet Psychiatry. 2015;2(3):271-274.
Saavedra D, Añé-Kourí AL, Barzilai N, et al. Aging and chronic inflammation: Highlights from a multidisciplinary workshop. Immunity & Ageing. 2023;20(25).
Marsland AL, Gianaros PJ, Kuan DCH, et al. Brain morphology links systemic inflammation to cognitive function in midlife adults. Brain, Behavior, and Immunity.2015; 49:31-38.
Emory Health Sciences. "How chronic inflammation may drive down dopamine and motivation." ScienceDaily. ScienceDaily, 4 June 2019.
Purnichi T, Rosca AE, Giurgiuca A, Pavel AN, Matei VP. Neuro-inflammation and its effects on cognition: A review of literature. Rom J Psychiatry Psychotherapy. 2018;20(3):100-103.
Xu Z, Knight R. Dietary effects on human gut microbiome diversity. British Journal of Nutrition. 2015;113(Suppl 1):S1-S5. doi:10.1017/S0007114514004127.
Johnson AJ, Vangay P, Al-Ghalith GA, et al. A guide to diet-microbiome study design. Frontiers in Microbiology. 2020;11:776. doi:10.3389/fmicb.2020.00776.

Your Ultimate Inflammation Reset.
Copyright © 2025 Optimal AF™ and Grey Fox Consulting, llc. All Rights Reserved
Follow us on social media:
DISCLAIMER: The information provided on this website is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read or heard on this website.
Facebook
LinkedIn
Youtube